Customized approach is based on specific job attributes.
Historically, most work involved physical labor, which results in physical fatigue that accumulates and dissipates progressively with time on and off work. Regulations focused on mitigating physical fatigue by prescribing the maximum length of shifts and the minimum duration of time off. Since WWII, huge growth has occurred in jobs that require cognitive labor, and mental fatigue, i.e., degraded or impaired cognitive as opposed to physical performance, has emerged as the primary concern for most industries. Evidence indicates that mental fatigue can accumulate not only from length of time awake and duration of time slept, but also the misalignment of work schedules with the biological clock. Therefore, tailored solutions that take this new evidence into account and move beyond prescriptive rule sets are required to mitigate such fatigue.
New evidence-based guiding principles co-published by the American Academy of Sleep Medicine (AASM) and Sleep Research Society (SRS) help employers design customized work shift durations. The principles consider a host of factors that lead to the accumulation of physical or mental fatigue, including length of time worked, duration of rest opportunity, time-of-day, job requirements, safety risks, lifestyle factors, and health. These principles include 1) assessment of potential risks, 2) a review of available countermeasures, and 3) a method to evaluate potential solutions using a risk-benefit tradeoff method, to create informed solutions that mitigate fatigue-related risks to health, performance, and safety.
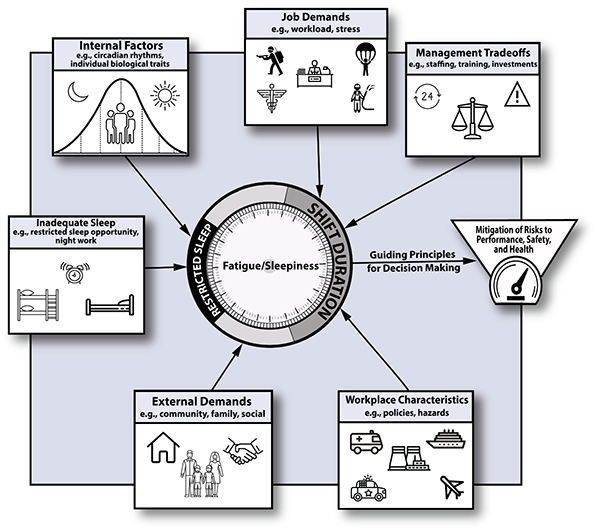
Risk factors that contribute to fatigue extend beyond hours work and length of time off between shifts, and include:
A broad set of tools and strategies are available to reduce or manage the risks associated with extended work shifts. They may aim to increase sleep (e.g., nap opportunities), improve alertness (e.g., strategic caffeine consumption), or mitigate outcomes (e.g., quality control checks, warning systems, and team-based work strategies). Countermeasures should be selected based on the assessment of the risks to be managed and require ongoing monitoring to identify opportunities for improvement.
To achieve effectiveness, the approach to decision-making often involves finding an optimal compromise between competing goals of many groups of stakeholders. The process should be scientifically informed, transparent, and inclusive of the various stakeholder groups; in particular, those whose lives and livelihoods would be directly impacted by changes to shift durations should be part of the decision-making process.
A variety of factors may increase or decrease shift duration-related health outcomes and impact safety and productivity. By assessing risks, considering countermeasures, and instituting an informed approach that considers trade-offs within an organization associated with the risks and benefits of various approaches, organizations can help keep employees healthy while meeting business goals.

About the author:
Dr. Indira Gurubhagavatula, MD, MPH, is associate professor of clinical medicine at the Perelman School of Medicine at the University of Pennsylvania, director of the sleep medicine fellowship at Penn, and director of the sleep disorders clinic at the Crescenz VA Medical Center in Philadelphia. Her work includes screening for sleep apnea in high-risk occupational settings. Dr. Gurubhagavatula has authored scientific publications and policy guidance for professional and governmental organizations regarding the management of obstructive sleep apnea in commercial drivers and has served as a consultant for federal organizations that address drowsy driving. She served as chair of the AASM Sleep and Transportation Safety Task Force, Occupational Sleep Wellness Presidential Committee, and Public Safety Committee; co-chair of the Work Shift Length Guidance Task Force; and presently serves as chair of the COVID-19 Task Force. Her work on these committees addressed key safety issues such as drowsy driving, school start times, daylight saving time, physician burnout, shift work, and mitigating the transmission of COVID-19 in sleep centers.
The paper providing the recommendations and the supporting scientific evidence, “Guiding Principles for Determining Work Shift Duration and Addressing the Effects of Work Shift Duration on Performance, Safety, and Health,” was co-published July 15, 2021, in the peer-reviewed scientific publications the Journal of Clinical Sleep Medicine and SLEEP.
As manufacturers offer more customization than ever before, managing product complexity has become a critical challenge. Tune in with Dan Joe Barry, Vice President of Product Marketing at Configit, who explores how companies are tackling the growing number of product configurations across engineering, sales, manufacturing, and service. He explains how Configuration Lifecycle Management (CLM) helps organizations maintain a single source of truth for configuration data. The result: fewer errors, faster quoting, and the ability to deliver customized products at scale.